The tradition in medicine was always to take a ‘history’ from the patient. The doctor would ask some simple ‘open’ questions and listen to the responses. (S)he would then ask a few highly directed ‘closed’ questions to elicit some important details and would then, as if by magic, announce a suspected diagnosis. Of course, the good doctor would then examine the patient to confirm the suspicions before giving treatment.

In the last half of the twentieth century, that started to change. We now have sophisticated machines that can look inside. Diagnosis has become immeasurably easier. We no longer operate just to explore, we now know with precision why we are making a cut into a patient and indeed, we even know exactly where to make the cut to minimise the risks (and over the last few years, we have discovered many ways to operate without even cutting through the skin at all).
But this comes at a risk. That risk is that we rely too much on machines to do the work for us. Whilst they bring enormous benefits to patients, the tradition of taking a history is starting to die. That is of considerable concern because doing unnecessary tests brings its own misery and suffering for patients as well as costs for the healthcare system. Take for example patients with symptoms of acid reflux. The standard investigation for this is an endoscopy. This test involves passing a tube with a camera on the end through the mouth into the stomach. Most people find this so unpleasant that they want to be made sleepy for the test. It involves having a dedicated unit with multiple staff to admit, monitor and help the patient recover after the procedure, not to mention the need for a sterile supply unit to ensure clean endoscopes. Endoscopy has become big business.
But what are we trying to detect? Well, cancer is obviously the most important pathology. Ulcers and bleeding are next. But everything else does not matter much, except for pre-cancerous conditions such as Barrett’s oesophagus. It is worth knowing if a patient has this because we can monitor and detect if the person is progressing towards developing cancer. If this happens, we can intervene to reverse the problem. One of the benefits of our new sophisticated machinery is that has made treating pre-cancer of the oesophagus a routine out-patient procedure rather than requiring surgery and a prolonged stay in hospital as it did only 10 years ago.
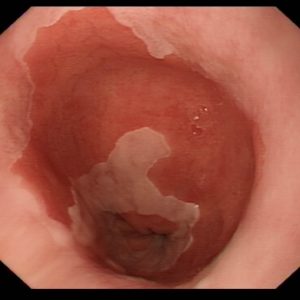
That is why we are so proud to have published this week our work on almost 2000 patients. See here. This shows that a very simple history – a set of questions along – will identify patients with Barrett’s oesophagus with an accuracy of over 80%. We have used the very latest ‘machine learning’ techniques to achieve this. This is far better than any previous research has ever managed to do. Complex science with a cool headed approach has led to a deceptively simple way to identify patients at high risk without invasive tests. Clearly, if the algorithm suggests that the patient does have Barrett’s oesophagus, we will still need to do an endoscopy to formally diagnose the condition. But if the test is really clear that the patient does not have the condition, they may be saved the discomfort and unpleasantness of having a test that is not needed.
We still need to validate our results in more patients groups. Once we have done this, we will still need to do endoscopy. But we will be able to target our interventions far more effectively. This will mean less patients undergoing procedures which turn out to be normal and more patients having tests that yield important results. Focusing our limited medical resources on those who need them most whilst saving those who don’t must be a good idea!







